In addition to a huge demand for advanced ventilators, the fight against the new coronavirus COVID-19 has also increased the need for Extracorporeal Membrane Oxygenation (ECMO), an approach that provides the body with oxygen when the lungs fail to perform this task. Getinge’s ECMO devices are designed to help keep critically ill patients alive while giving their damaged lungs time to recover.
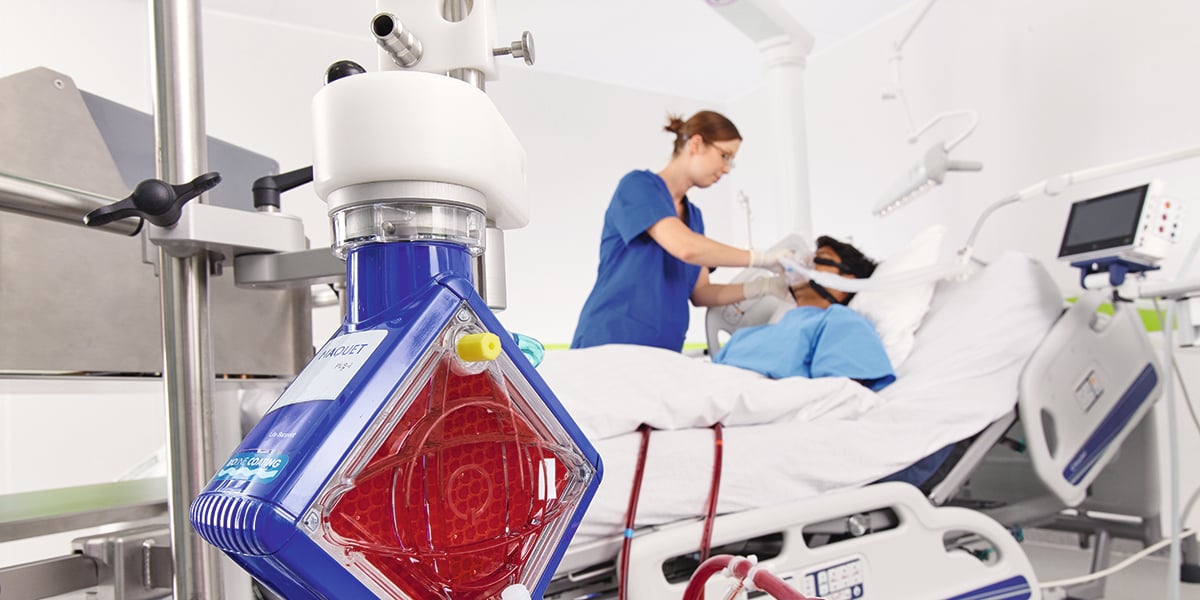
Severe symptoms of COVID-19 often leads to respiratory failure and pneumonia1. Some patients also develop Acute Respiratory Distress Syndrome (ARDS). When the lungs are no longer able to provide sufficient oxygen to the body, even with the help of mechanical ventilation, using ECMO is a potentially life-saving alternative.
The method has also been used in previous serious flu epidemics, such as the swine flu, and it is recommended by the World Health Organization (WHO) as a treatment for promoting recovery in the most serious cases of COVID-19.
“ECMO itself will not cure a patient, but the technology is designed to help doctors gain valuable time to save lives. A patient can be connected to ECMO for weeks, but the reported average time for COVID-19 cases is 10 days according to the Extracorporeal Life Support Organization (ELSO2),” says Stefan Schied, Product Manager at Getinge. “These COVID-19 patients are in such critical conditions that ventilation and medication are not enough to keep them alive. With ECMO, the doctors gain time to take the right measures and it gives the patients lungs time to heal,” Stefan Schied says.
This is how it works
Depending on configuration, ECMO can be used for lung support (as in the case of COVID-19) and it can be used for both heart and lung support. ECMO replaces the lung function by oxygenating the patient’s blood outside the body.
“Blood containing a low amount of oxygen and a high concentration of carbon dioxide leaves through a catheter inserted into a large vein. It connects to an oxygenator that adds oxygen and removes carbon dioxide,” explains Stefan Koch, Getinge’s Head of Training and Simulation Cardiopulmonary. He continues:
“As long as the patient’s heart is able to pump sufficiently, the freshly oxygenated blood can be returned to the veins. This procedure, which is called VV-ECMO, is used in cases of severe acute respiratory diseases.”
When the patient’s heart fails and can’t effectively deliver blood to the body, the returning blood ‘bypasses’ the heart and pumps directly through a large artery (VA-ECMO).
Getinge’s product portfolio
Our broad, high-end product portfolio includes a choice of devices and consumables to provide individual and sufficient extracorporeal heart and/or lung support, such as centrifugal pumps, oxygenators, heater units, tubing sets, and catheters and cannulae.
Cardiohelp is one of the world’s smallest portable heart-lung support systems, weighing 11.5 kilos and easily carried by one person. The Cardiohelp System is approved for air and ground transport.
“The difference between our system and the other competitors is the compactness and integration. This simplifies transport and the general handling of the system and also has fewer challenges during use for the user,” Stefan Koch explains.
The HLS Set Advanced oxygenator is specifically developed for VV-ECMO and VA-ECMO extracorporeal life support for up to 30 days (CE region). Powered and monitored by Cardiohelp, it combines user-friendliness with approvals necessary for use when transporting patients within the hospital or in-between hospitals.
Getinge’s second ECMO alternative, the Permanent Life Support (PLS) system, consists of the Rotaflow Console, Rotaflow Drive and the PLS Set; a pre-connected standard set consisting of the PLS-i oxygenator and the centrifugal pump RF-32 incorporated into a tubing set. It fulfills the demanding requirements for extended application time up to 14 days.
Learn more about Getinge’s ECMO solutions >>
This information is intended for an international audience outside of the U.S.
[1] Clinical management of severe acute respiratory infection (SARI) when COVID-19 disease is suspected Interim guidance 13 March 2020. WHO reference number: WHO/2019-nCoV/clinical/2020.4
[2] COVID-19 Cases on ECMO in the ELSO Registry. ELSO Organization (https://www.elso.org/Registry/FullCOVID19RegistryDashboard.aspx) accessed May 19, 2020.