Mechanical ventilation – the most used short-term life support technique worldwide for patients that cannot breathe on their own – is a key component in the ongoing fight against the new coronavirus COVID-19. Already since the early 1970’s, Getinge has provided the global medical community with state-of-the-art solutions for ventilation in critical care.
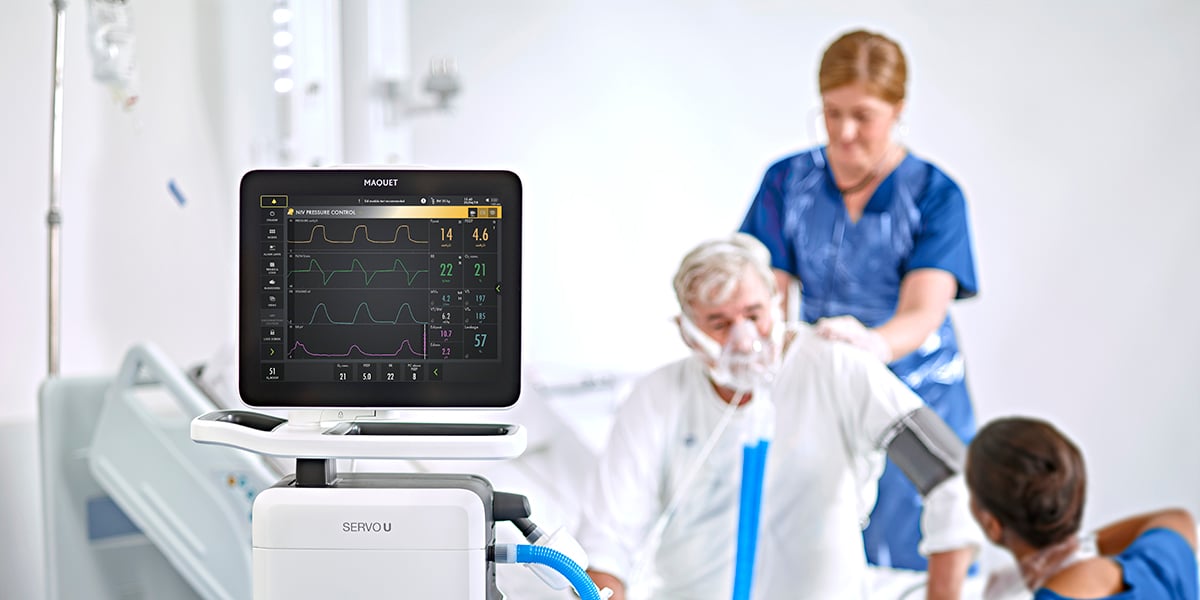
Modern ventilators can effectively take over the patient’s breathing function. Mechanical ventilation does not heal the patient but enables him or her to remain stable during treatment, while the underlying process necessitating mechanical ventilation is resolving.
The respiratory support can be adapted to physiological needs in order to protect the patient from worsened lung injury, respiratory muscle dysfunction, and lung infection. As soon as clinically indicated there should also be a transition to spontaneous breathing to minimize risk of increased morbidity and mortality. Weaning is the process of removing the patient from mechanical ventilation where optimization of patient-ventilator synchrony is of outmost importance.
Mechanical ventilators are very advanced devices; carefully designed to be effectively operated by trained clinicians in a hospital’s intensive care unit (ICU) under stressful conditions.
This is how it works
Mechanical ventilation can either be invasive, via a tube in the airways, or non-invasive through a face mask or nasal prongs. It also differs from how we breathe on our own.
During natural breathing, the diaphragm as the main respiratory muscle contracts, and the chest-wall expands. This creates a negative pressure that pull air into the lungs. When the respiratory center orders the breathing muscles to relax, the air leaves the lungs passively.
A ventilator is designed to deliver a mechanical breath to the lungs until it reaches a user-selected criterion, which can be based on time, flow, volume or the patient´s own neural respiratory activity. Once the lungs have been filled as intended, the inspiration stops, and expiration starts.
Using a mask is generally preferred as it maintains the body’s natural barrier for getting infections into the lungs. However, in many cases the patient’s condition will require intubation, for example when it comes to severe lung injury or disease.
For patients with severe impairment of oxygenation (e.g. ARDS), it is important to use a ventilation strategy that has the potential to improve patient outcomes and optimize the benefit-to-cost ratio for lungs, heart and the respiratory muscles. An example of such a strategy is the assessment of lung recruitability, in order to choose ventilator settings that regains lost effective lung volume and at the same time does not cause over-stretching of alveoli, the small cells in the lungs responsible for gas exchange.
The history of Servo-u
Getinge’s first Servo ventilator, Servo 900, was introduced in 1971 and started a revolution in intensive care ventilation. Way ahead of its time, this small, silent and efficient electronic ventilator, with a feedback system for controlling gas delivery, enabled the clinician to reliably achieve the targeted volumes and respiratory rates intended for the patient.
 Today, all ventilators in the Servo family are designed to optimize the interaction between patient and ventilator for better comfort and performance.
Today, all ventilators in the Servo family are designed to optimize the interaction between patient and ventilator for better comfort and performance.
The latest generation features many options for protective and personalized ventilation. The aim is to contribute to better outcomes by helping the individual patient breathe while avoiding complications and weaning him or her off the ventilator earlier.
Ventilator Management of critical illness due to the coronavirus, COVID-19
Although the majority of people with the coronavirus COVID-19 have uncomplicated or mild illness, some will develop critical illness and will require mechanical ventilation. The most common diagnosis in severe COVID-19 patients is severe pneumonia1.
Personalized lung protection with Servo-u
Servo-u brings many options for personalized lung protection and weaning. Availability of different functions may differ pending on market. For more information, see the Getinge website.
Learn more about Getinge’s mechanical ventilators
Servo-u is a trademark of Maquet Critical Care AB.
[1] Clinical management of severe acute respiratory infection (SARI) when COVID-19 disease is suspected Interim guidance 13 March 2020. WHO reference number: WHO/2019-nCoV/clinical/2020.4