Mechanical ventilation is a life-support treatment for patients that are not able to breathe on their own. But mechanical ventilation can also cause complications. Therefore, Getinge is continuously working on solutions to support clinicians in their daily practice to enable protective ventilation strategies for the patients.
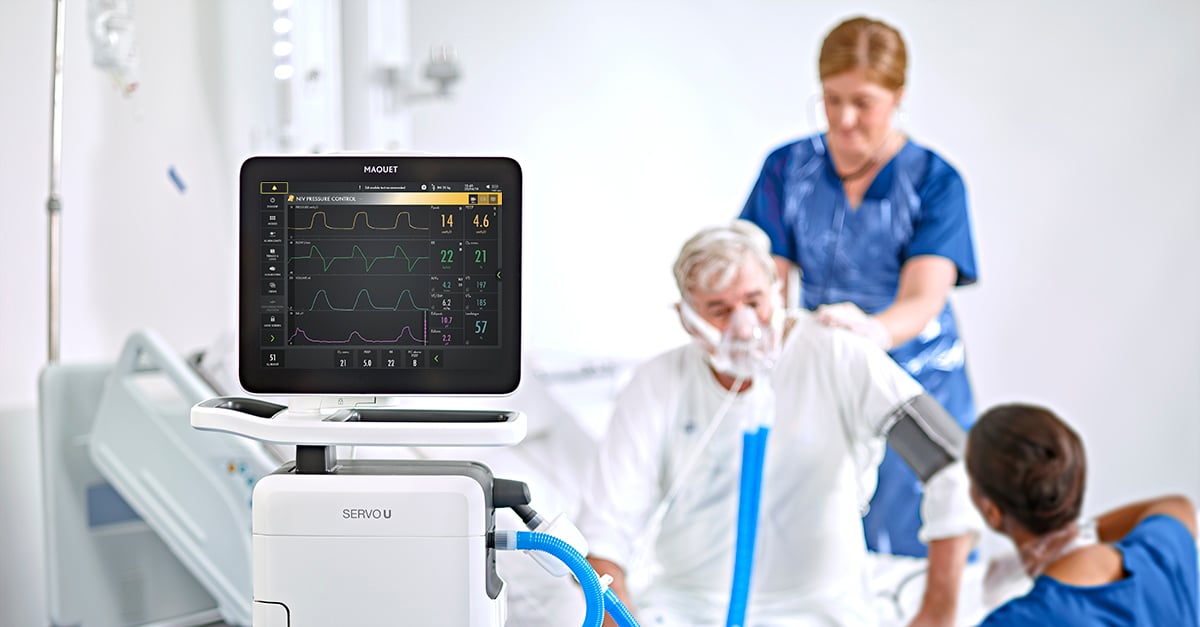
Severely ill patients who need support from a ventilator are cared for in a hospital’s intensive care unit (ICU). Mechanical ventilation can either be invasive, via a tracheal tube in the airways, or non-invasive through a face mask or nasal prongs. It differs from how we breathe on our own.
Over the last decades, awareness of the potentially adverse effects of mechanical ventilation has grown, triggering the key question: Can ventilation strategies make a difference for maintaining gas exchange while avoiding complications, such as lung injury, pneumonia, or diaphragm dysfunction?
Clear visualization is important for the user
Protective ventilation strategies proposed as standard of care are prescribing low tidal volumes (the amount of air delivered to the lungs in each ventilator breath) related to the patient’s predicted body weight and limited driving pressures and plateau (the pressure applied to the small airways and air sacs in the lungs).
“Clear visualization of driving pressure and tidal volumes on the ventilator is very important for helping clinicians to detect changes and verify potential lung injury.” says Dr. Miray Kärnekull, Medical Director at Getinge.
The first Servo ventilator, introduced in 1971, featured a feedback system for controlling gas delivery that revolutionized ventilation in intensive care. Now Getinge offers customers a wide range of ventilators with easy-to-use tools and interfaces that contribute to better patient outcomes by helping clinicians to reduce complications and wean patients off the ventilator earlier.
The latest generation of Getinge’s groundbreaking Servo-u features many effective options for protective and personalized ventilation.
Opening collapsed lung regions
“Our aim is to provide solutions that support the clinicians in their lung protective ventilation strategies says Helena Stone, Global Training Manager at Getinge. “One example is our new Open Lung Tool (OLT) which aims at re-expanding previously collapsed lung regions with a brief and controlled increase of the transpulmonary pressure. This helps clinicians to perform lung recruitment maneuvers in a safe and easy way.”
Neurally Adjusted Ventilatory Assist (NAVA) is another intelligent functionality which promotes spontaneous breathing by using measurements of the patient’s own respiratory drive to deliver a personalized ventilatory support.
Getinge’s product range also includes the Servo-n ventilator for premature babies. It has shown to increase comfort and lower the need for sedation, which may allow more sleep and greater energy for growth and maturation. It is able to ventilate babies as small as 300 grams; providing them with the breathing support they need while protecting the lungs, brain and other developing organs.
Read more about Getinge's solutions for mechanical ventilation